By Jackson Okata
Nairobi, Kenya — Drastic cuts in donor funding are likely to curtail Kenya’s decades-long progress in the fight against HIV. Already, effects of reduced funding, particularly from the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR), whose annual budget to Kenya has been slashed by nearly 50% from USD 58.7 million in 2024/25 to USD 29.9 million in 2025/26, are being felt.
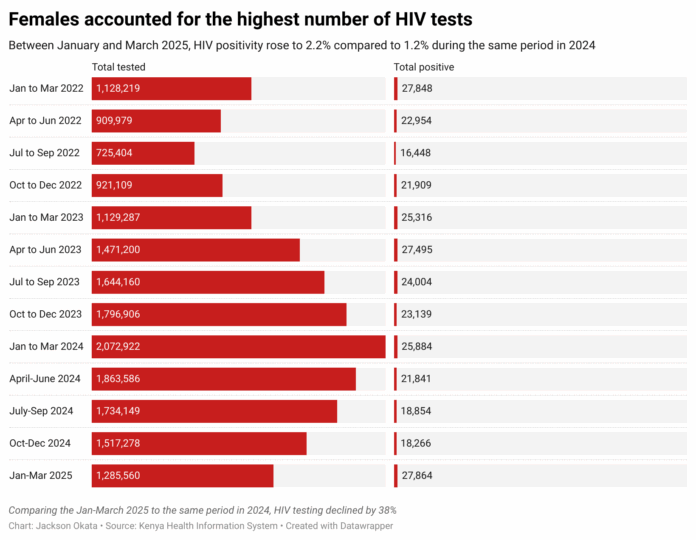
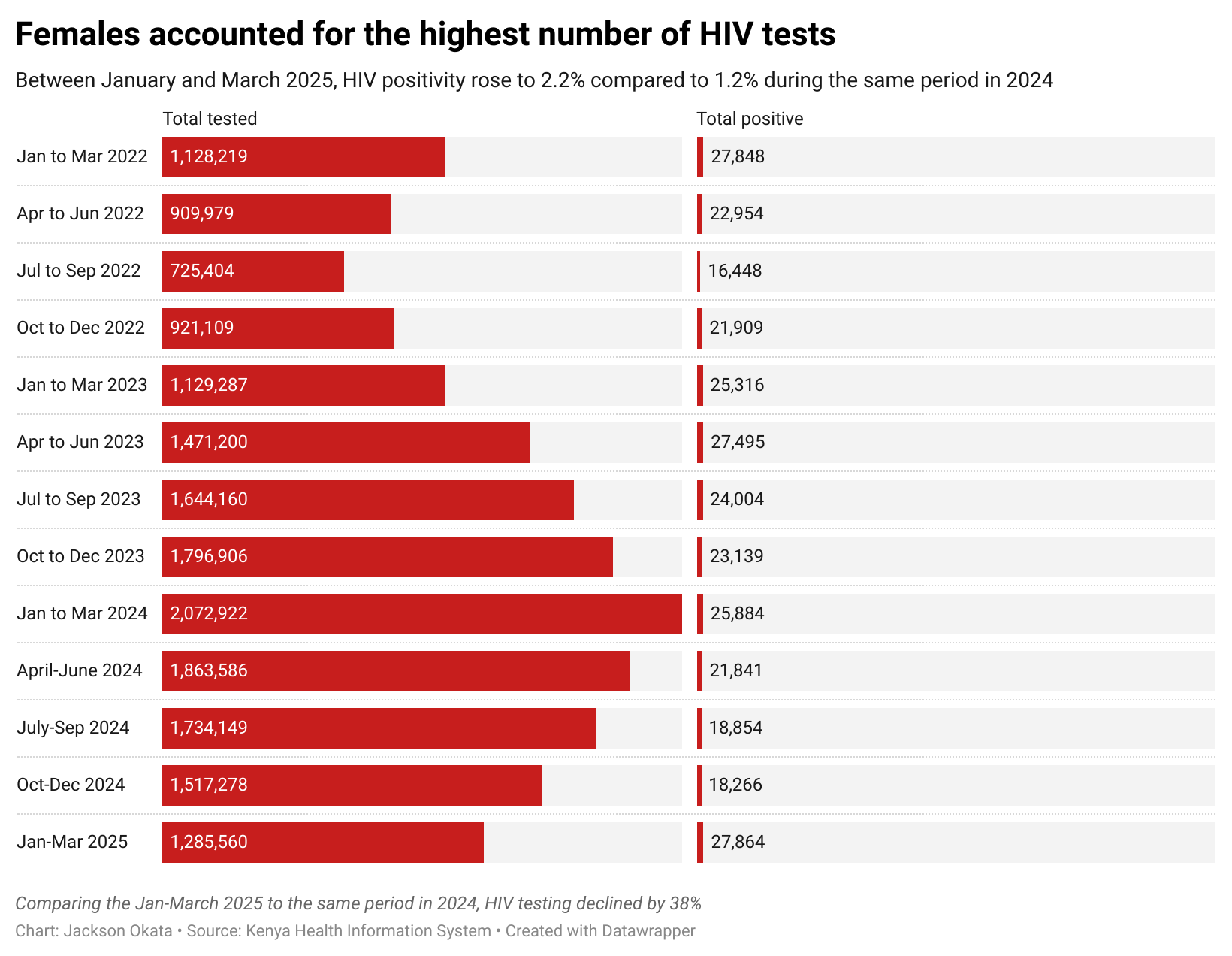
Data from the Ministry of Health shows a troubling drop in HIV testing and prevention uptake. Between January and March 2025, HIV testing declined by 38%, with only 1.28 million people tested compared to 2.07 million in the same period in 2024.
Females aged above 10 years accounted for 76% of all HIV tests conducted between January and March 2025.
The country recorded an increase in HIV positivity, which rose to 2.2% in early 2025, up from 1.2% in 2024.
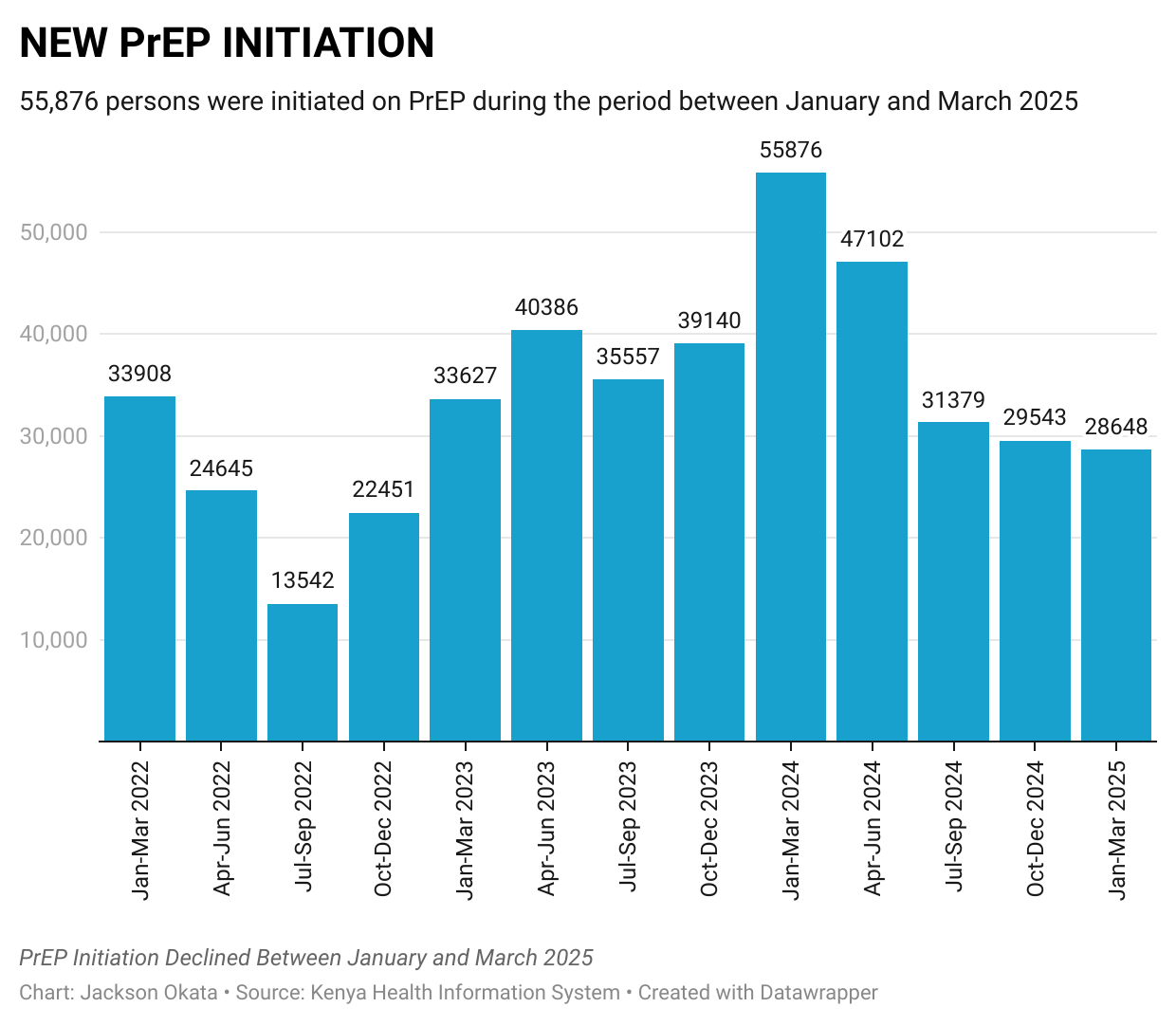
More worrying is the decline in the uptake of Pre-Exposure Prophylaxis (PrEP) by 49%. During the period, 28,648 people were initiated on PrEP, down from 55,876 during the same period in 2024.
Patriciah Jeckonia, programs officer at LVCT Health, Kenya, says, most HIV prevention programs, including the DREAMS initiative and key populations (KP) programs, have either been paused or defunded, and focus has shifted to delivering only the most essential services to those already living with HIV.
With Kenya recording 16,752 new HIV infections in 2024, Jeckonia expresses fear that the number could rise if prevention gaps are not urgently addressed.
“All facilities offering ART are currently operating at reduced capacity, and donor-funded health workers have been laid off, creating an acute shortage of human resources for health”, Jeckonia said.
According to UNAIDS, while short-term commodity availability has improved in Kenya’s health facilities, the loss of donor-supported staff has hampered service delivery.
In its new report, AIDS, Crisis and the Power to Transform, UNAIDS noted that Kenya anticipates no stockouts for the next three to six months, but raised concerns about long-term sustainability if staffing gaps remain.
Kenya has set targets to eliminate AIDS in children by 2027 while aligning with global UNAIDS targets to end AIDS as a public health threat by 2030. Another impact of the funding cuts is the suspension of Kenya’s Health Information System (KHIS), which captures and reports national HIV program data. This has paralysed the country’s ability to track trends, plan interventions, or assess performance.
In a bid to sustain HIV and STI prevention activities, UNAIDS, in collaboration with the National Syndemic Diseases Control Council, is developing a funding proposal targeting the China International Development Cooperation Agency.
In December 2024, the Ministry of Health launched a national sustainability plan for the HIV response, emphasising the integration of HIV services into broader health services across all public facilities.
Kenya’s HIV interventions over the decades have been effective, with the country’s prevalence dropping to 3.31%, with 95% of people living with HIV knowing their status.
UNAIDS says that although HIV programs remain relatively well funded in Kenya, investment in HIV prevention interventions is slow, with only 8% of HIV funding allocated to prevention.
Globally, UNAIDS warns that an additional six million new HIV infections and four million AIDS-related deaths could occur between 2025 and 2029 if US-supported HIV treatment and prevention services collapse
“This is not just a funding gap. It’s a ticking time bomb,” said UNAIDS Executive Director Winnie Byanyima at the launch of the organisation’s 2025 global AIDS update on Thursday.
UNAIDS data shows that in 2024, 630,000 people died from AIDS-related causes, 61% of them in sub-Saharan Africa, with over 210,000 adolescent girls and young women aged 15—24 acquiring HIV.