|
Getting your Trinity Audio player ready...
|
By Melisa Mong’ina
Nairobi, Kenya: On a chilly evening in the heart of Nairobi, Caren Awino sits quietly, her voice carrying both strength and exhaustion. At just 48, her life tells a story of resilience against illnesses that have drained her health and reshaped her family and future.
“I was diagnosed with hypertension when I was just in my twenties. I used to attend a clinic at a Health Center with elderly patients who constantly questioned my presence, because it was believed that it only affected the old,” she recalls.
At the time, Caren was young and did not understand why her condition was uncontrollable, despite changing from one prescription to another. Years later, during the COVID-19 pandemic, another devastating blow followed.
The signs had been there all along. It was only after being admitted at Kijabe Hospital that the doctors confirmed she had lived with undiagnosed type 2 diabetes for years. Her blood sugar was extremely high so she was immediately put on insulin.
“I was diagnosed in 2019. At first, it was hard to accept. I cried a lot because I didn’t know how to go about it and managing both conditions required a lot of money,” Caren shares.
Caren was hospitalised for three months and placed on oxygen because alongside hypertension and diabetes, she was also battling bronchitis, lung complications, and was overweight.
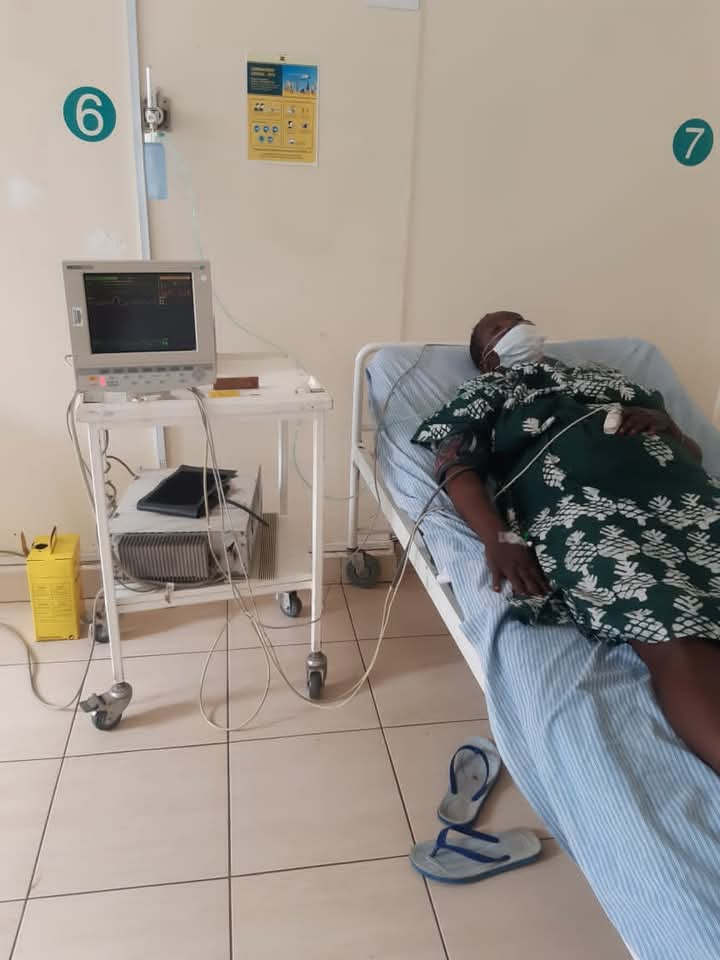
A nutritionist introduced a strict meal plan to help her lose weight and stabilize her blood sugar.
“They told me to avoid carbohydrates, reduce proteins, and eat more vegetables. But the diet is expensive. Even today, it is expensive,” she explains.
Due to her determination, she managed to lose 30 kilograms, stopped insulin, and switched to oral medication. However, the struggle still persisted as she often requires at least 1,000 shillings for medicine every month, a sum she cannot always raise. At times, she is forced to skip medication due to financial burdens.
“I was supposed to lose 70 or 80 kilograms. I eventually reached 90 kgs. Sometimes I might skip medication due to financial issues. When that happens, my vision blurs, and I become weak. Since I can’t afford all the proper meals, I just eat whatever I have to survive,” she says.
Abandoned at Her Weakest And The Broken Promise of Health Coverage
Caren’s health struggles also tore her family apart. In 2019, while still admitted at Kijabe hospital, her husband abandoned her. He couldn’t bear watching her in such a critical condition nor handle the hospital bills that kept piling up.
“My husband saw me dying, injecting myself, and the bills rising. He had also lost his job during that period. He couldn’t bear it, so he left,” she recalls. “After being discharged from the hospital, I went home and found him gone.”
Her two children, then in their twenties, stepped in to help, by doing small jobs to provide food and rent. Caren often feels like a burden to them. At times, they could also lament about her condition, advising her to seek other alternatives.
“I usually find it difficult asking them for money all the time. I feel I’m a burden. Sometimes they also complain that they are tired of my conditions, suggesting that I should find another way to get help. This breaks me a lot since I have no other options,” she says, her voice heavy with pain.
Caren survives on a paltry 3,500 shillings from stipend that often comes late, sometimes after several months. This delay worsens her financial struggles, making it difficult to afford medication and maintain her diet.
Although she has registered with the Social Health Authority (SHA), she says it offers little help for people with chronic illnesses like hers.
“With SHA, it’s hard to get medicines from private hospitals. They usually refer us to Kenyatta or Mbagathi hospital. But I often lack transport money to go there,” she explains.
Even at the Health Centre patients are rarely able to access the medicines they need.
“There are no medicines in this health centre. We used to have free medical camps for diabetes, but nowadays there is nothing. When they come, we are told to purchase medicines at a fee, yet many can’t afford,” Caren says.
A Plea for Women Living With Chronic Illnesses
Caren’s voice carries the frustrations of many women in low-income areas battling chronic illnesses. She wishes for a healthcare system that does not abandon the sick.
“My prayer is that the government considers us, those with chronic illnesses,” she says. “Even in rural areas, women are suffering. You can’t buy food and medicine at the same time. The little you get, you eat, so that you don’t collapse.”
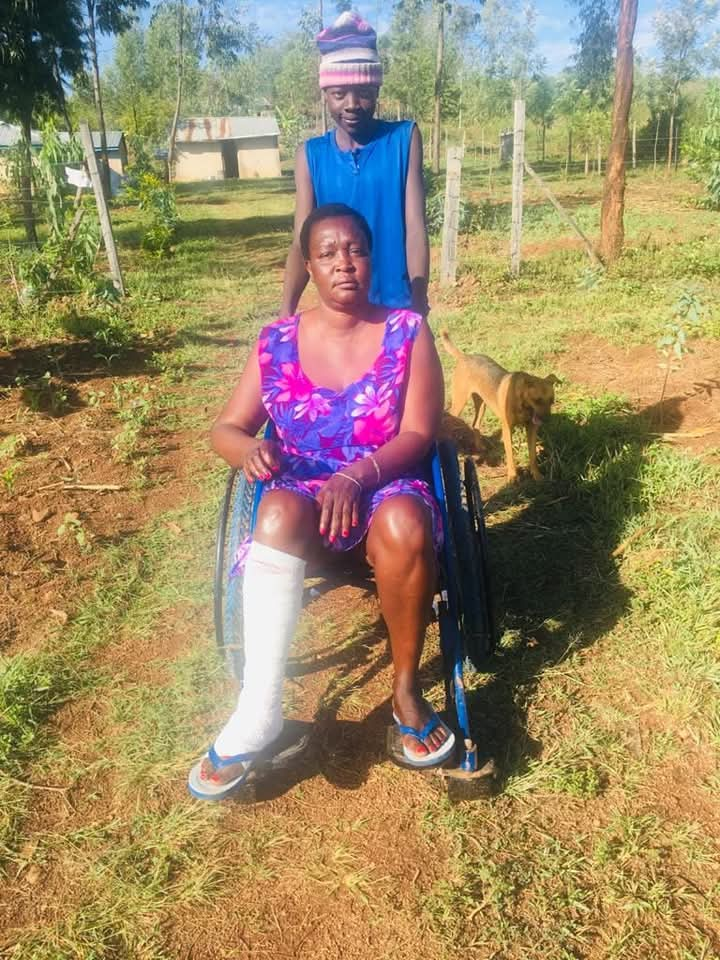
Her journey grew even heavier in August 2024, when she was diagnosed with breast cancer, compounding her pain and financial strain.
“It still bothers me because it has spread to the other breast. Although I’m on medication, this condition also needs money which I don’t have,” she explains.
As she shares her story, she hopes it will shine a light on a crisis that has been ignored for too long.
“I have really gone through a lot,” she says. “But I want people like me to be heard, feel loved, and cared for. We are really suffering. But maybe if people hear us, help will come. We should not be suffering in silence. Our cries need to be heard.”
A Patient Advocate View on Advocacy and Gaps in Health Care Systems
To understand the broader challenges within Kenya’s health system, particularly for women living with non-communicable diseases (NCDs), we spoke with Evans Majau, Chairperson of the National Caucus of Patient Led Organizations on NCDs in Kenya and a board member of NCD Alliance Kenya.
As someone who has walked alongside patients and caregivers, witnessing the daily struggles of women and families living with NCDs in Kenya, Majau highlights how inequality often leaves women like Caren fighting for survival.
“The obstacles are layered. For women in Kibera, Mathare, or in rural counties like Turkana and Marsabit, the barriers are clear: affordability, ignorance, availability, and awareness. Essential medicines are often out of stock, facilities are distant, and when drugs are available, the cost is overwhelming,” Majau explains.
He adds that women’s responsibilities and the pressing financial burden make it even harder for them to prioritise their own health. A mother may choose between buying hypertension/ diabetes medicine or buying unga for her children.
Majau further stresses that poverty has turned manageable conditions like hypertension and diabetes into life-threatening diseases, trapping families in cycles of illness and financial crisis.
“Women are caregivers, mothers, sometimes sole breadwinners. Seeking treatment isn’t just a health decision; it means weighing whether to miss a day’s income or put food on the table,” says Majau.

Adding “I’ve listened to countless women describe how they stretch out their pills, taking half doses or skipping altogether. Some even turn to herbal alternatives, traditional healers, not because they prefer them, but because it’s all they can afford.”
Although the government launched the Social Health Authority (SHA) to increase access to care, Majau says the gaps remain significant. He acknowledges that the scheme is a welcome policy shift but it’s uneven in practice.
“In some urban and peri-urban settlements, access through SHA-accredited clinics has improved. Yet in rural areas, women still travel 30–40 kilometers for care because contracted hospitals that offer primary care and outpatient services are few. For families earning less than 300 shillings a day, even bus fare becomes a challenge,” he observes.
He further points out that the problem with SHA is implementation gaps as many women are enrolled but don’t understand how it works, what’s covered, where to go, or how to claim them. Others find facilities out of stock of essential medicines or are asked to pay extra fees despite being insured.
“All this erodes trust and hope. Many women in informal work or in remote areas remain outside the system altogether. We often hear the heartbreaking refrain: We have registered but we don’t get the medicine we need. Why should we embrace SHA?” Majau warns.
For meaningful progress, he emphasizes the need to strengthen primary healthcare by equipping local facilities, ensuring a reliable supply of essential medicines, and training more health workers. He also underscores the importance of community awareness and accountability.
“We need strong community-level education so that women know their rights and how to navigate SHA. Patients, especially women, must be part of monitoring and giving feedback. Finally, we must remember that health does not exist in isolation: without food security, safe transport, or decent incomes, insurance alone cannot meet women’s needs,” he stresses.
He concludes with calls to policy makers, practitioners, and advocates, urging them to ensure that women’s voices are heard.
“The women we meet every day are resilient, resourceful, and full of dignity,” Majau reflects. “They do not want handouts; they want fairness and a real chance at life. Our duty is to ensure that no woman in Kenya ever has to choose between buying food for her children and buying her medicine.”
A Health Expert’s View on NCDs and Women’s Access to Health Care
According to Dr. Catherine Karekezi, Executive Director of NCD Alliance Kenya, the crisis of non-communicable diseases (NCDs) in Kenya is far from abstract. It is a daily reality she encounters through women like Caren, who are fighting for their health with little more than courage and prayer.
“Conditions like diabetes and hypertension are lifelong. They don’t pause while you look for money to buy medicine. They demand daily care, and when that care is missing, the consequences are severe, kidney failure, amputations, and heart attacks. The real tragedy is that preventing these complications is far cheaper than treating them,” she observes.
For women, the struggle is even heavier. Dr. Karekezi explains that mothers often sacrifice their own health for their families. Many skip clinic appointments or cut back on medication to stretch household budgets for food and other household needs.
“Women frequently have limited access to healthcare and face higher exposure to NCD risk factors because of gender norms and economic pressures. A mother may know her blood sugar is unstable, but she will stay at her market stall because the day’s income is what ensures her family eats. Her life takes second place,” she explains.
Women with NCDs also lack access to healthy nutritious diets that they require to manage their condition because of financial constraints.

In many households, men still control financial decisions, leaving women with little say in when or how to seek treatment. Widows and single mothers, like Caren, are forced to shoulder both financial and emotional burdens on their own.
“In traditional households where women depend on male partners, their access to timely diagnosis and routine follow-up is often restricted. This dependency can delay care, worsening their condition,” Dr. Karekezi notes.
Stigma adds another layer of difficulty. Some women avoid checkups out of fear of shame, while young mothers hide high blood pressure during pregnancy to escape judgment. Insufficient knowledge and skills among mid-level health professionals further compounds the challenges.
“Pregnancy-associated NCDs like high blood pressure or gestational diabetes are leading causes of poor outcomes for mothers and children. Yet many young women, especially teenagers, conceal their conditions because they fear stigma from families and communities,” she explains.
Environmental and commercial risks also weigh heavily on women. In informal settlements, smoke from charcoal and firewood fills tiny one-room homes, exposing women and children to respiratory and cardiovascular diseases. Meanwhile, tobacco and alcohol industries aggressively market harmful products to women and girls.
“Air pollution from solid fuels significantly increases the risk of chronic respiratory and heart diseases. At the same time, industries target women with tobacco, nicotine, and alcohol products, worsening an already heavy burden,” she laments.
Although policies like the Social Health Authority (SHA) were designed to close these gaps, Dr. Karekezi admits that on the ground, progress is uneven. Clinics frequently lack basic medicines and diagnostic equipment, and women enrolled in SHA still find themselves turned away or asked to pay extra.
“SHA is meant to provide treatment and care at primary health facilities at no cost to the patient. But the reality is different. Patients who have complications are required to seek care at higher-level facilities, which are not easily accessible and often demand out-of-pocket payments. For vulnerable women, this creates an almost impossible barrier,” she says.
She stresses that unless SHA and similar policies become gender responsive, the cycle of inequity will continue. Women must not only be recognised as beneficiaries but should be engaged as key stakeholders in policy discussions and implementation of SHA.
“Stock-outs of medicines and supplies, out-of-pocket costs, and weak supply chains undermine women’s care. Women are an economically active part of society. If they are not healthy, we undermine families and the nation as a whole. Healthy women are essential for Kenya’s progress,” she adds.
Dr. Karekezi emphasizes the need for stronger screening services, reliable supplies of medicines, and psychosocial support for those living with NCDs.
“Primary facilities need to offer screening for diabetes and hypertension, be stocked with medicines, and have health professionals trained in management of such NCDs. Communities must be aware that diabetes and hypertension are manageable with early diagnosis and follow-up. Patients should know why medicines matter even when they feel well, and how to manage their diet and physical activity. Living with a chronic condition also affects mental health, so we need counselling services, support groups and safe spaces for sharing and learning,” stresses Dr. Karekezi.
Through the NCD Alliance Kenya, women’s voices are being placed at the center of the response through county advocacy chapters.
“We have started support groups and NCD county chapters where women with NCDs, and those championing the cause, can learn, share, and raise their voices. These groups empower women to manage their conditions, improve family nutrition, and influence health policy,” says Dr. Karekezi.
Caren’s story is not unique. Across Kenya, many women especially in rural and low income areas quietly carry the burden of chronic illnesses without adequate medical support.
Medicines are scarce in public facilities, private hospitals remain unaffordable, and health insurance often leaves them uncovered. Through support groups and advocacy chapters, many women have gathered the courage to raise their voices, hoping that their cries for help will not be in vain.














