|
Getting your Trinity Audio player ready...
|
By Mary Mwendwa
Nairobi, Kenya: I was in a work meeting when my phone lit up with her name at 3:00 PM. Excusing myself, I answered to a stranger’s voice: “Hello, I am Doctor… from Kenyatta University Referral Teaching and Research Hospital. We suspect your daughter has Mpox.”
The air left my lungs. Mpox. The word echoed with everything I knew: its contagious nature, the stigma, the global outbreaks I’d reported on.
The doctor on the phone, sensing my stunned silence, softened his tone. He explained they were referring her at Mama Margaret Uhuru Hospital-KNH for confirmation. “Please do not panic. Even if positive, she mainly needs isolation. It has progressed for days, which means it’s not an immediate life threat.”
His words were a lifeline of logic in a rising tide of panic.
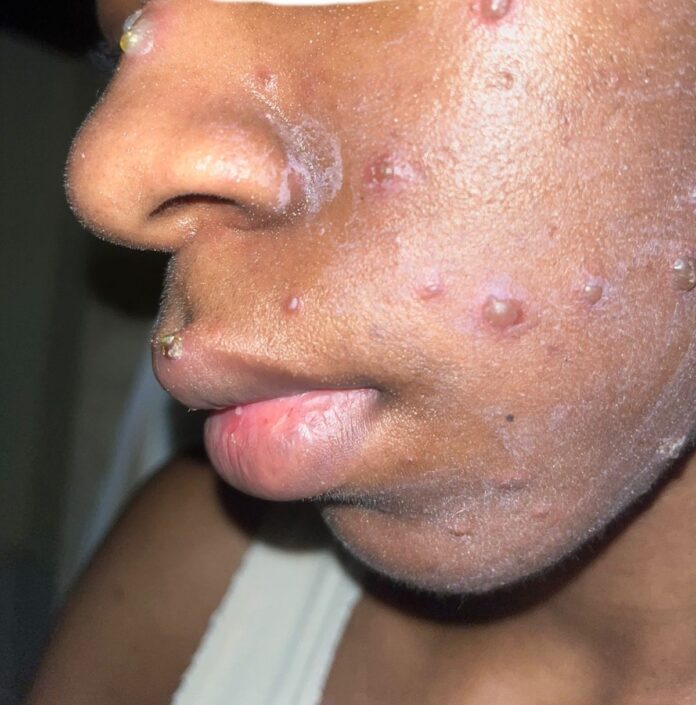
When I reached my daughter, her voice was thin with fear. “Mum, they kept saying ‘It’s the one… It’s the one.’ They looked scared. They checked my back and the swollen nodes.” Her description was a chilling confirmation. In Kenya, while case numbers are relatively low, the medical community is on high alert, aware of its potential spread. The coded language and palpable anxiety in the hospital spoke volumes about the fear this disease still carries.
Rushing to join her, I received another call. The clinical voice was unequivocal: “Confirmed. The classic signs are all there.” The message was devastating. By 7:30 PM, as Nairobi darkened, the doctor advised me to turn back. My daughter was being sent home in a taxi. Our new reality was isolation and a terrifying vigil for symptoms in the rest of the family.
My heart hammered against my ribs. I cancelled everything—an editor’s convention in Kilifi, all assignments. The professional was fully consumed by the personal.
It had begun a week earlier. My daughter had woken with a rash we both dismissed as chicken pox. She felt chills and a fever. We went to a private facility, Guru Nanak Ramgarhia Sikh Hospital. Despite our active Social Health Authority (SHA) insurance, we were told it wasn’t accepted that day and paid in cash, a minor inconvenience amid our worry.
The doctor confirmed our assumption: chicken pox. We were sent home with painkillers and the ubiquitous calamine body lotion. For days, we followed the routine. But after five days, instead of improving, the lesions intensified into painful, raised bumps. Her fever would spike menacingly at night, and then came the swollen lymph nodes—a telltale sign, in my professional capacity, I knew was not typical of chicken pox. It was the first cold trickle of dread. We agreed she must see a specialist at a government referral hospital.
Even as I pen this story, I am still in a state of quiet shock, grappling with the surreal reality of how this disease connected my professional and personal lives. The month of November has been the most challenging for my family and me.
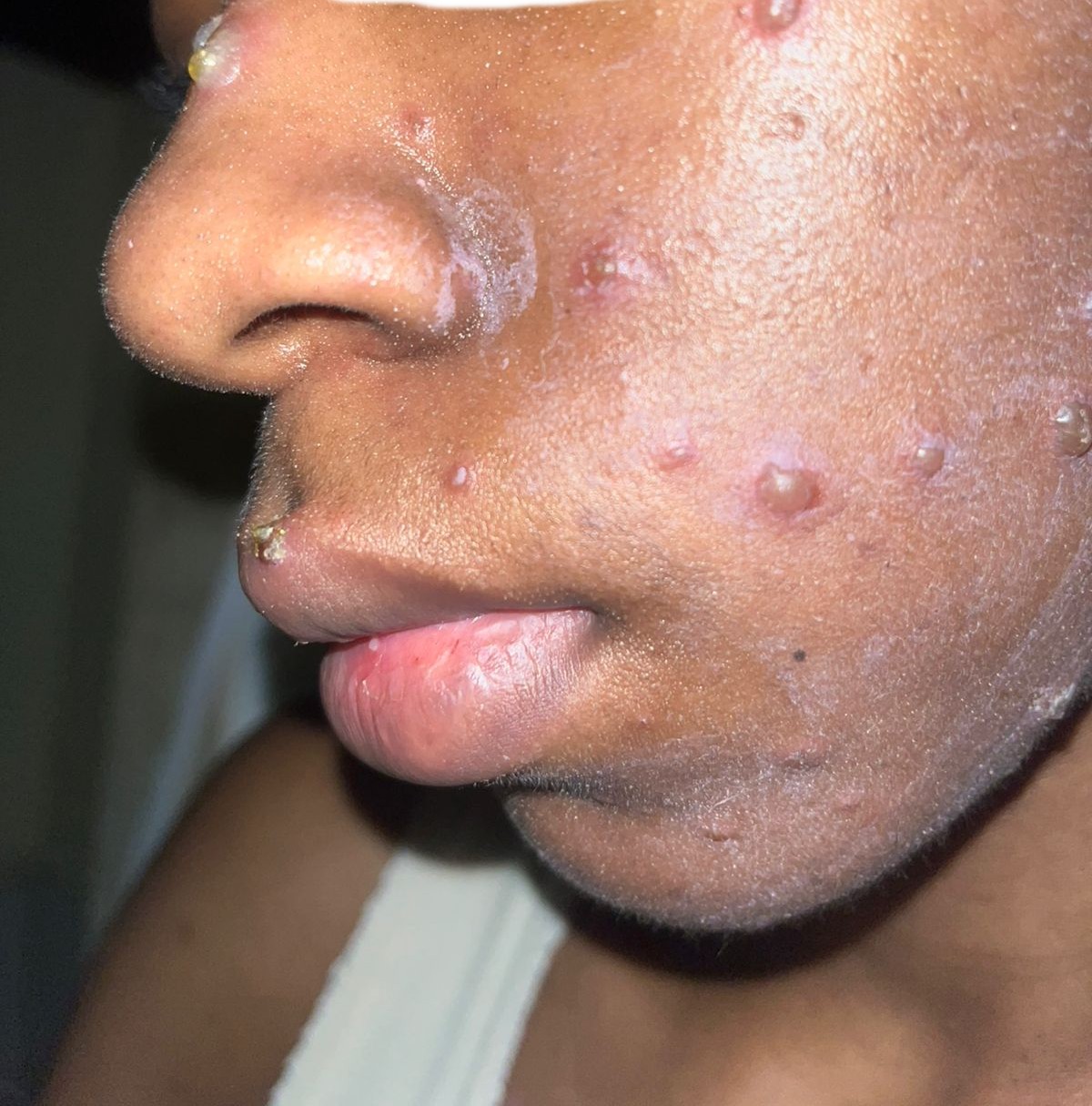
As a health and science journalist, this year has been one of profound observation. I have reported from hospital wards, witnessing the raw struggle for breath. I have tracked disease vectors to their hidden habitats, all to translate complex realities for you, the reader, to understand that even uncommon diseases can unleash havoc and claim lives. This, however, is my most intimate account: the story of how Mpox stopped being a headline and became our lived nightmare.
I have written news articles about Mpox and filed away press releases from organizations like Médecins Sans Frontières, those steadfast front-line responders. I never imagined that the clinical facts and figures would one day include my daughter.
My daughter is in her final year at a university here in Kenya, passionately studying AI and Software Engineering. I am the sole frequent traveler in our home due to my work. This chapter began just after I returned from Kilifi, where I was with a team visiting the KEMRI-Wellcome Trust Research Programme in Kilifi, a trip focused on understanding health threats, ironically now mirrored in my own living room.
The Crash Course in Caregiving
I plunged into research, but now every fact was personal and chillingly specific. According to the Ministry of Health, Kenya had recorded just over 20 confirmed cases since the global surge began, with a handful of suspected fatalities under investigation. The numbers were “low” from a national perspective, but utterly devastating when your family becomes a statistic.
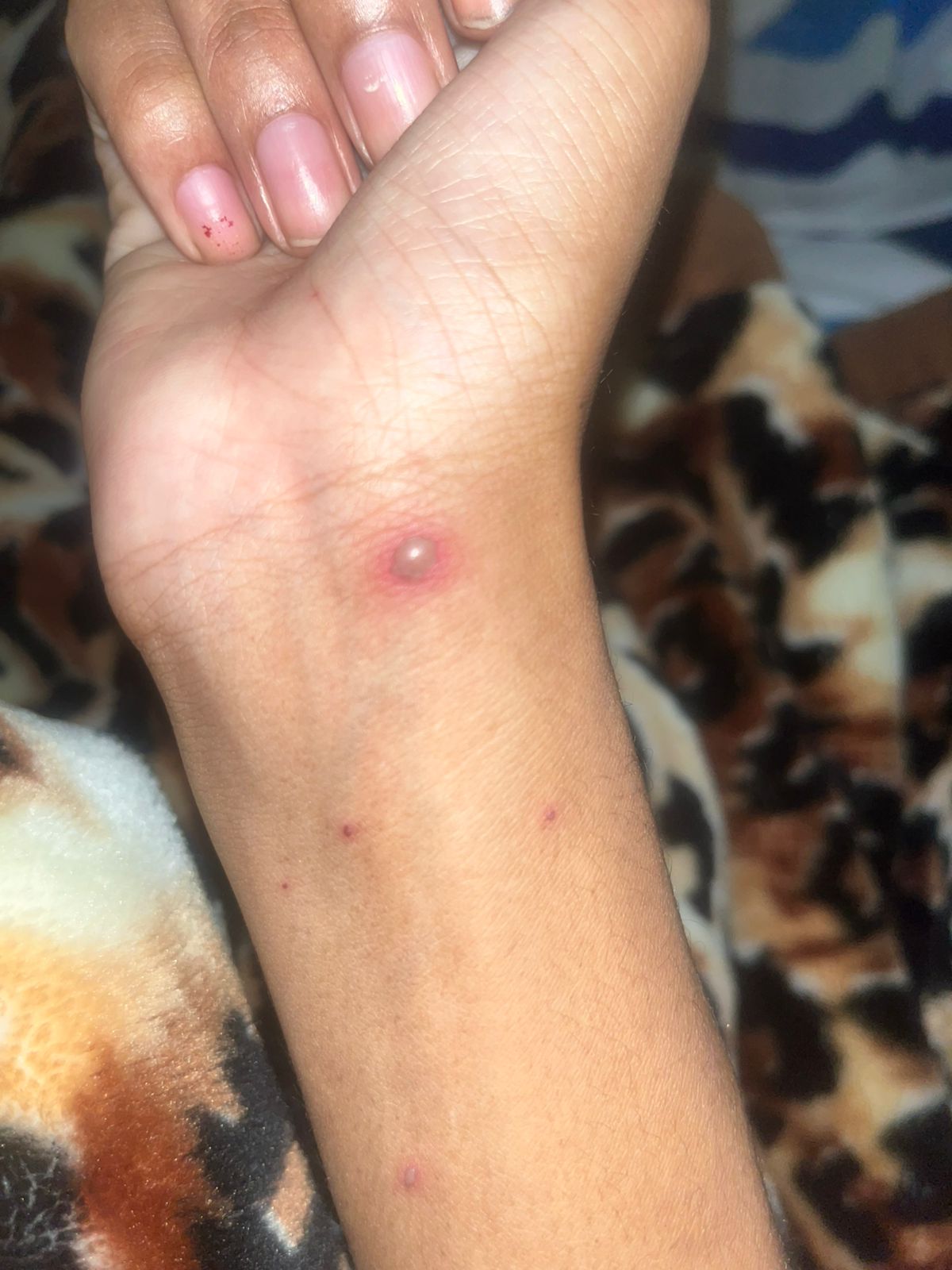
Globally, the 2022-2023 outbreak saw over 90,000 cases and 150 deaths, with a case fatality rate historically between 1-10%, depending on the strain and access to care. The current global strain, thankfully, has shown a lower lethality, but for the vulnerable, the threat is real.
Mpox spreads through close contact, infected fabrics, and body fluids. The signs my daughter showed were textbook. The most haunting question: Had we already exposed everyone? Where could she have gotten it? The doctors said it was likely from an unidentified community transmission. Kenya has had cases in Nairobi, Mombasa, Kisii, and Uasin Gishu, a spread showing it was no longer an imported curiosity but a circulating threat.
There is no specific antiviral for Mpox, but supportive care and vigilance against secondary bacterial infections are critical. An antiviral, Tecovirimat, and a vaccine, MVA-BN, exist but are largely inaccessible here, reserved for severe cases or outbreaks in high-risk groups.
Our treatment plan was isolation, pain management, and time.
We transformed our home. One bedroom became an isolation ward. I was no longer just a mother; I was a caregiver in gloves, a comforter from behind a mask, a fear manager for us both. Telling my traumatized daughter, “It will be okay,” required a strength I had to fabricate on the spot. I was offering comfort, but I desperately needed to hear myself.
This experience has been a brutal teacher. As a journalist, I understood Mpox as a public health challenge. As a mother, I felt its profound personal terror—the anxiety that stretches silence in a hospital corridor, the weight of isolation, and the fierce hope that follows every fading lesion.
My daughter is now recovering well; her lesions have dried. We are hopeful, forever changed, and profoundly aware that diseases know no boundaries; they can touch any life, any family, even a journalist who thought she was just telling the story.