|
Getting your Trinity Audio player ready...
|
By Jackson Okata
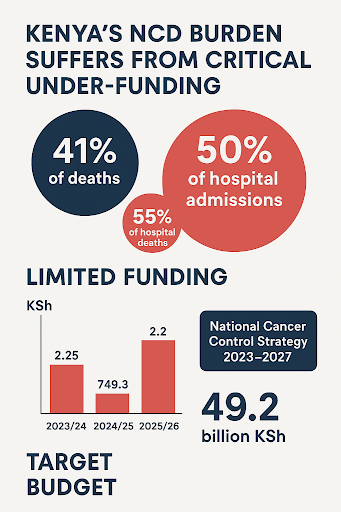
Nairobi, Kenya- Non-communicable diseases now account for over 41% of all deaths in Kenya, with cancer leading as the top contributor. Still, limited funding directed to the fight against NCDs can only be described as a public health disaster.
According to the Kenya Health Policy Survey (2014-2030), NCDs account for 50% of hospital admissions and 55% of hospital deaths in Kenya.
Prisca Githuka, Board Member of the Kenya Network of Cancer Organisations (KENCO), notes that there is a dangerous disconnect between Kenya’s health budget priorities and the actual burden of diseases like NCDs.
“Funding of the health sector is not just about resources. It’s a matter of justice, equity, and human rights”, Githuka told Talk Africa.
Kenya’s NCD funding remains limited. For instance, the National Cancer Control Strategy (2023–2027) calls for KSh 49.2 billion, yet less than 10% has been availed.
In the financial year 2023/2024, the treasury allocated KSh 2.25 billion for NCD funding, with the figure reducing to KSh 749.3 million in FY 2024/25, before rising again to KSh 2.2 billion in FY 2025/26.
Thomas Lindi, CEO of the Kenya Tobacco Control and Health Promotion Alliance (KETCA), says the funding instability makes it impossible to plan or deliver services effectively.
“NCDs are a real burden on our health system, and funding should be consistent and aligned with the rising disease burden,” said Lindi.
Lindi argues that the government should be bold enough and implement 70% of tobacco excise taxes as per the WHO recommendation to both curb harm and raise revenue that can then be used in Ring-fencing funding for NCD programs.
Gershim Asiki, a research scientist at, African Population and Health Research Centre (APHRC), blames the gap in the funding of NCDs on the lack of a dedicated budget line and ring-fenced financing for NCDs.
“Unlike HIV, we do not have a dedicated budget line for NCDs, and during the budgeting process, the sector gets lumped together with others, which leads to funds diversion in some cases’’ Asiki said.
Asiki warns that the NCDs burden will continue to worsen unless stakeholders put more investment in preventive measures as opposed to treatment.
“There was a lot of global attention that was put on HIV, and resources were put into prevention, which is what should happen with NCDs”, Asiki said.
Ahmed E. Ogwell Ouma, a global health diplomacy expert, says that underfunding for NCDs isn’t just numbers but poor health outcomes.
“When such a critical sector is underfunded, we are talking about late diagnosis, escalating treatment costs and deaths that we could as well prevent with the right funding”, he said.
And with limited funding, families are being plunged into poverty as they grapple with expensive NCD treatment and management.
Dr Catherine Karekezi, Executive Director of NCD Alliance Kenya, says NCDs reduce household incomes by 28.6% with low-income households being the most affected.
“NCDs are life-long conditions which require regular follow-up and may damage body organs if not well controlled”, said Dr Karekezi.
Ouma says there is heavy reliance on out-of-pocket spending in NCDs management and treatment, with households bearing nearly a quarter of healthcare costs, pushing many into financial hardship.
Kenya has set ambitious targets of raising its total health budget to 5% of GDP and 15% of the national budget by 2030, as well as allocating 35% of county budgets towards health by the same year. The Abuja Declaration recommends allocating at least 15percent of national budgets to health, while the WHO urges a minimum allocation of 5% of GDP.













