|
Getting your Trinity Audio player ready...
|
By Melisa Mong’ina
Nairobi, Kenya: Non-communicable diseases (NCDs) such as diabetes and hypertension have long been thought to be afflictions for the elderly. But today, the landscape is changing as more young Kenyans face the reality of living with these chronic illnesses.
Living With Type 1 Diabetes: The Young Warrior
It’s been five years since Rashid Mohamed’s diagnosis. His journey began in high school in 2021. Initially, the school nurse treated him with painkillers, but still his symptoms persisted, so he went home for more tests.
“I experienced symptoms like frequent thirst and constant hunger. I couldn’t sleep at night due to frequent urination, and the school nurse only gave me painkillers, which didn’t help. I decided to go home for more check-ups,” recalled Rashid.
His uncle took him to a doctor friend who checked his sugar levels, which were dangerously high. They gave him first aid and took him to the hospital the next day.
“I never expected things to be serious, but when my uncle’s doctor friend checked me, the blood sugar was extremely high. They only conducted first aid on me, then I was transferred to Msambweni hospital the next morning,” he adds.
He never imagined having the same condition as his grandmother. It was hard for him to adjust to a strict diet and daily medication.
“I had witnessed how management was a challenge to my grandmother. The transition to a strict diet and daily medication was hard for me. Sometimes, I could get tired and depressed due to the new lifestyle,” says Rashid.
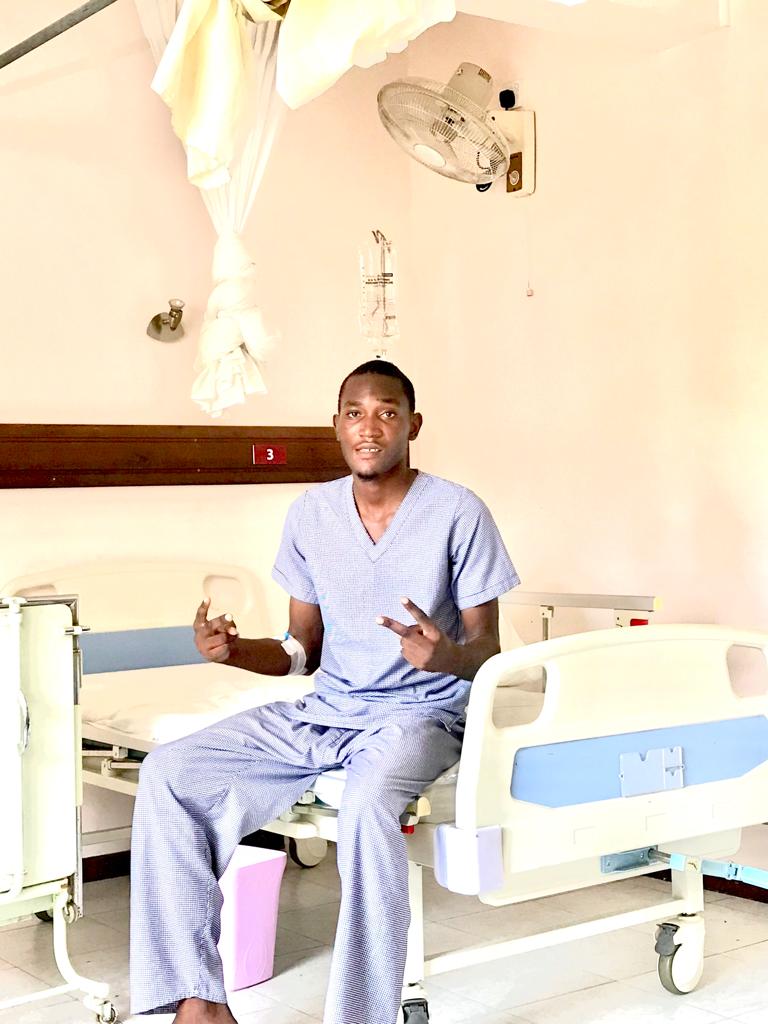
At school, the principal allowed him under certain conditions. He later began reading about diabetes and met with people who had the same condition. Together, they formed a community-based organization called the Youth Diabetes Champion.
“Going back to school was a challenge, but after talking to the school director, I resumed, though with signed conditions. I did more research and networked with people with similar conditions. We later formed a CBO to assist in creating awareness about NCDs,” he explains.
Most of the support came from his father and uncle. At school, he informed friends so that they would be able to assist in case of emergencies.
Rashid explains how access to medication has been challenging even with an active and paid Social Health Authority (SHA).
“Access to medication is hard since some hospitals lack the drugs while others require me to pay out of pocket, yet my SHA is often paid for and activated,” adds Rashid.
His group advocates for NCD programs even in schools to raise awareness among young people.
“We lack enough awareness and support, particularly among young people. Since we started this CBO in 2019, finding donors to support our projects has been one of our biggest hurdles,” he explains.
In 2025, they were able to get support from NCD Alliance Kenya which boosted their advocacy efforts. He also encourages young people to accept the condition as it is the key step to proper care.
“We are grateful for the support we received from NCD Alliance Kenya, and we hope to get more partnerships to push our advocacy agenda further,” says Rashid. “To my fellow youths, acceptance is crucial, particularly in treatment and management.”
Josephine’s 20-Year Journey of Strength: Battling Type I Diabetes
Josephine Gitahi was only 12 years old when she found out she had type 1 diabetes. The cost of insulin, syringes, and tests made life difficult.
“Diabetes is a disease of numbers; you can’t control what you don’t measure. Monthly tests like HbA1c, eye and kidney checks are costly since SHA doesn’t cover them,” she explains.
She experienced signs such as fatigue, rapid weight loss, blurred vision, frequent thirst, and urination.
Her lifestyle changed. She now eats small portions and engages in daily exercise as part of the treatment.
“I now eat in moderation depending on the insulin units. I also avoid junk and try to engage in daily exercises. This has made me more responsible,” she says.

Josephine stresses the need for early detection to both young people and adults, acknowledging the crucial support network she has had in her journey.
“Early detection helps prevent both short-term and long-term diabetes complications. The care I received from family, friends, and groups like YoungnSweet and the Diabetes and Hypertension Clinic (DHC), have helped me a lot,” adds Josephine.
She highlights that many young people, especially the unemployed, still face significant gaps in awareness and support for managing type 1 diabetes.
“While progress has been made, mortality rates have increased due to insufficient awareness and support for youths living with type 1 diabetes, particularly the unemployed,” she emphasizes.
Josephine urges young people living with diabetes to live fully. “Diabetes should never be a limiting factor, just live your life to the fullest. It is not a disease but a manageable condition. It becomes a disease if unmanaged.”
Diagnosed as a Teenager: Andrew’s Journey With Type 2 Diabetes
Andrew Adams was in Form 4 preparing for his final year exams in 2009 when he began feeling unwell. He had dizziness, joint pain, frequent urination and thirst, and blurred vision. He was wrongly given malaria drugs at school. His condition worsened until he went home.
“I visited the school dispensary and was given malaria drugs, but they didn’t help. I decided to go home. On the way, I kept asking the driver to stop so I could relieve myself,” he says. “The passengers didn’t understand my condition and told the driver to keep going. I had to hold it the whole 30 km from Mbita to Homa Bay.”
At home, he was rushed to the hospital where the doctor revealed he had type 2 diabetes. Adams was admitted for two months and had to work extra hard to catch up with revision.
“My parents lived in Ndhiwa, and I was studying at Mbita High School. I stopped at my aunt’s place in Homa Bay. At the county hospital, my blood sugar was extremely high. I was admitted for two months and discharged with insulin. This made me study extra hard since I was far behind with revision,” he explains.

Now, Adams ensures that his insulin stays cool when traveling and also carries diabetic-friendly snacks.
“Managing diabetes is hard because of the cost of insulin, syringes, and suitable foods. I rarely interact much at work,” he adds.
He struggled with changes in weight and appearance, and social isolation. He hides his condition to avoid discrimination.
“Strict routines, body changes, and social isolation overwhelm me. It’s also hard using public transport or being in long meetings. I avoid telling some of my colleagues that I have diabetes to escape their judgments. I usually say I have allergies,” he shares.
Adams credits his mother and siblings for their support, urging young people to take control of their health.
“My mother and siblings have been supportive. Diabetes isn’t a death sentence. Watch your diet, exercise, and learn more about your condition,” says Adams.
Tabitha’s Story Living With Type 2 Diabetes as an Adult
Tabitha Ndung’u, a mother and a caregiver, found out she had type 2 diabetes during the COVID-19 pandemic at the age of 45.
She had been feeling tired, losing weight, and urinating often before getting tested at a local chemist.
“I noticed unusual signs. A doctor at a chemist confirmed I had type 2 diabetes. It was a shock, I never thought it would happen to me,” she says.

As a sweet tooth person, adjusting to a strict, costly diet and daily medication routine was a hurdle. Mood swings and emotional stress followed, especially due to her rapid weight loss. With time and proper care, she adjusted to her new life.
“I used to snack on chocolate after work, so adjusting was hard. Managing diabetes is expensive, and the mood swings affected how I related with people. But eventually, I adjusted to this new life,” she adds.
Her family had limited knowledge of diabetes. She only got support from a few friends and colleagues who understood her condition.
“I had a few colleagues who understood my condition and supported me in this journey. I’ve never gone for any tests with my family. I think they felt like it was just a normal disease. They didn’t know it’s a lifelong condition,” says Tabitha.
She believes there’s little awareness about diabetes among both the young and old. She calls for more awareness, urging everyone to eat healthy, get tested often, and not to lose hope after diagnosis.
“Many people don’t understand diabetes. It’s a silent killer, you may not notice until your health worsens. If you have it, accept it, take your medication, eat well, and exercise. If you don’t, avoid junk food, stay hydrated, and get checked regularly,” urges Tabitha.
Young and Hypertensive — Milliscent Resilience
Many people think high blood pressure (hypertension) only affects older people, but more young people are now being diagnosed.
Milliscent Akinyi was just 32 when she found out she had high blood pressure, after suffering from strong headaches and dizziness. She had to make many changes with her diet.
“I used to feel dizzy, severe headaches, numbness on my legs and at times I collapsed. I no longer eat wheat products and fatty foods like before. Now, I eat a lot of fruits and vegetables, I exercise a lot, and take less sugar and salt,” explains Milliscent.

She often faced stigma from friends. The doctors and nurses used to question her condition since it was believed to be a disease of the old.
“My self-esteem went down at some point as I was starting my medication. The doctors and nurses used to ask me where I got this elderly disease from. This also applied to my friends. It has taken me two years to accept myself,” she shares.
Purchasing the right foods is difficult. This makes her pressure rise. Accessing treatment has also not been easy, especially if one isn’t financially stable.
“My pressure usually spikes due to stress whenever I lack money to purchase the required foods. Treatment isn’t easy or hard. One has to be financially stable to get the required treatment,” she adds.
Her family offers little support, but she has few friends who are always by her side. For colleagues, none is aware since she fears stigma.
“I don’t feel supported by my family, few friends have been there for me. I have not informed anyone at my workplace because I fear getting stigmatising words from them,” Milliscent says.
She clears out some of the myths she has heard about hypertension, explaining that it can be genetic and it can affect anybody regardless of their age or status.
“This condition can be inherited and it starts by itself. It can get anyone,” she says.
She adds that the government does not give enough attention to chronic illnesses. Only a few small organizations help, and they don’t have enough money to reach everyone.
“In Kenya, NCDs are not in the priority list of the duty bearers. We lack enough awareness and support from the government. The only people who offer support are a few CSOs but they cannot reach many people due to inadequate finances,” explains Milliscent.
Beatrice’s Battle and Advocacy Journey
Beatrice Opany, a caregiver to a child living with sickle cell disease and also a health advocate for people with chronic illnesses, has been living with hypertension for four years. Her journey began with a health scare at work.
“I was shocked because I knew that hypertension was only for old people. Before collapsing, I had a persistent headache, feeling dizzy, fatigue, and shortness of breath,” she narrates.
Beatrice had to stop drinking coffee and reduced salt intake. She often feels very tired at times. Learning about the dangers of high blood pressure made her more anxious.
“I now have to watch what I eat. I don’t drink coffee as much as I used to. I also avoid taking salt. Sometimes I just feel tired and exhausted. After diagnosis, my anxiety increased, especially after knowing the health outcomes like heart attacks and stroke,” she says.

Caring for her child, especially during sickle cell crises, makes her pressure rise even more. Her husband, who also has high blood pressure, and her colleagues at work have been supportive.
“In my case, the condition was triggered by stress. Managing it has been difficult because whenever my child has a crisis, the blood pressure rises,” Beatrice explains.
“I have strong support from my spouse, who also lives with the same condition. At work, most of my colleagues are aware, and whenever I’m unwell, they allow me to go home and rest.”
She says getting treatment was easier under NHIF, but now with SHA, she has to pay from her pocket, which is very expensive.
“Accessing treatment was better when we had NHIF, but nowadays with SHA, it’s worse because I have to do it out of pocket, which is extremely expensive, especially since we are three people living with NCDs under one roof,” she says.
Beatrice urges young people to be careful, eat well, and do regular blood pressure check ups.
“Our young people should know that it is a silent killer and it affects any age group. They should eat healthy, do a lot of exercises, and at least do a regular monitor of their BP because for some people, it doesn’t show symptoms,” urges Beatrice.
She also wants people to stop believing common myths, encouraging those living with NCDs to keep fighting because with proper management one can live well.
“A lot still needs to be done in terms of awareness. To people living with any NCD, it’s not the end of life. We can still live a long life as long as we follow the doctor’s directions and take our medication,” she emphasizes.
As these long-term illnesses continue to affect more Kenyans, young and old, health experts are calling for early testing, better education, and stronger support for young people to manage their conditions and live healthy lives.
Understanding Blood Sugar — Expert’s Insights
Dr. Catherine Karekezi, Executive Director of NCD Alliance Kenya (NCDAK), explains that glucose, primarily derived from metabolised carbohydrates, is the main source of energy for the body.
“The body has a mechanism of maintaining balance in the body. Glucose is the primary energy source and comes from the food we eat, especially from carbohydrates. For glucose to enter the body cells and produce energy, a hormone called insulin allows it to move from the blood into the cells,” explains Dr. Karekezi.

She adds that diabetes is a condition linked to how the body regulates blood sugar.
“Diabetes is a condition where the blood glucose levels are higher than they should be. This happens either because the body is not producing enough insulin or the insulin produced is not working properly. It can also be a combination of both,” she says.
She explains that lack of enough insulin hinders glucose in entering into the cells to produce energy. This causes symptoms like fatigue, frequent urination, and sometimes one may also feel very hungry.
Why Diabetes and Hypertension Are Rapidly Rising Among the Youth
She outlines the two main types of diabetes. Type 1 occurs when the body does not produce insulin, requiring patients to inject it to survive. In contrast, with type 2 diabetes, the body still makes insulin but not enough, or it does not work effectively.
“People with type 1 diabetes cannot regulate blood glucose because their bodies do not produce insulin, and it must be injected. Unlike type 2, it cannot be prevented,” she says.
“In type 2 diabetes, the insulin produced is insufficient or ineffective. Treatment may start with tablets that improve insulin use, but some people eventually need injections,” adds Dr. Karekezi.
Dr. Karekezi adds that blood pressure is the force exerted by blood in the blood vessels as the heart pumps blood throughout the body.
“Blood pressure is important because it allows blood, which carries oxygen and nutrients, to reach all the organs,” she says.
“However, when blood pressure is higher than normal the heart muscles strains a lot causing complications like heart failure and stroke.”
Further, she notes that aging, lifestyle choices, and family history play a role in increasing the risk of type 2 diabetes and high blood pressure.
“Unhealthy diets, physical inactivity, alcohol and tobacco use, air pollution, and stress increase the risk of these conditions. While family history is also a contributor, many cases can be prevented through lifestyle changes,” she explains.
She highlights the difference between traditional healthier lifestyles, and today’s modern eating habits which are more high in fat, sugar, and salt, but low in nutrients.
“Traditionally, people were more physically active and ate healthier diets with minimal salt, sugar, and oil. Today’s lifestyle, with more processed foods, contributes to the rise of type 2 diabetes and hypertension, particularly among young people,” explains Dr. Karekezi.

She emphasizes that imbalance between the energy consumed and the energy used increases the risk of chronic illnesses.
“We are eating a lot of high-energy food but are not physically active. The unused energy is being converted and stored as fat leading to overweight, obesity, increasing risk of diabetes, and hypertension,” she stresses.
She observes a worrying trend in the eating habits of young people today, describing it as dangerous.
“Young people often order fast foods, which are high in salt, fat, and sugar. Many now prefer using microwaves instead of traditional slow cooking methods which take more time.” she adds.
Dr. Karekezi says physical inactivity is also on the rise due to increased dependency on motorbikes (boda bodas), sedentary jobs, and screen time increasing the risk of non-communicable diseases.
“We no longer walk as much as we used to due to the presence of boda bodas. At work, people sit all day using laptops and phones. Lately, unhealthy diets are much cheaper than the healthier options, so people buy what they can afford,” she highlights.
Air pollution is also a growing concern, especially in areas where many people use charcoal or firewood to cook in homes with poor ventilation. Stress from life struggles also increases the risk of disease.
“There’s also the issue of stress due to various reasons. Air pollution has worsened, especially in informal settlements where the houses are poorly ventilated and most people use charcoal or biofuels for cooking,” says Dr. Karekezi.
Fighting Misconceptions and Filling Awareness Gaps
Dr. Karekezi debunks the misconceptions surrounding who is at risk for hypertension and diabetes.
“There is a common perception that these diseases only affect older people. Many, particularly young people believe they are not at risk and avoid going for check-ups at medical camps,” she points out.
She encourages health professionals to shift their perspective on these conditions as they can affect any age group.
“Healthcare workers were also under the impression that these were conditions of older persons. This has changed. Now, they need to understand that anyone can get hypertension or type 2 diabetes, especially those who are overweight,” urges Dr. Karekezi.
She points out that Kenya’s new health insurance cover, SHA, is failing to meet the needs of people with chronic illnesses, leaving patients vulnerable as they are asked to pay out of pocket, which most cannot afford.
“Most patients pay out-of-pocket for treatment which is very expensive, especially for those with low income. Many cannot access the care they need even with their SHA insurance,” she explains.
Why Awareness and Policy Support Matter
Lack of proper management of non-communicable diseases like hypertension and diabetes might result in serious damage to other organ systems.

“If non-communicable diseases like hypertension and diabetes are not managed properly, they can lead to serious complications in other organs, which are difficult and expensive to treat,” she says.
Dr. Karekezi stresses the need to educate young people about the risk factors as a crucial part of prevention efforts.
“Increasing awareness of diabetes and hypertension helps people understand the risk factors so that they can make healthier lifestyle choices to prevent or delay the onset of these conditions,” emphasizes Dr. Karekezi.
She highlights ongoing efforts to equip Community Health Promoters (CHPs) with practical tools to help screen people in villages and refer those at risk to hospitals.
“CHPs now have glucometers and blood pressure machines which helps them screen people in the community, identify those at risk and refer them to the nearest hospital for further care,” she explains.
Religious leaders also play a crucial role in promoting health awareness in churches and mosques.
“Religious leaders in churches and mosques are important in spreading awareness. They can invite health professionals to educate the congregants about non-communicable diseases,” she says.
Health-focused events such as medical camps and screening days are crucial in providing access to free or low-cost health services to the public. Dr. Karekezi also highlights the importance of including physical activity in school curriculum.
“Health days have medical campaigns which offer opportunities for free or affordable screening. We also need to reintroduce physical activity in schools to help children stay healthy and prevent NCDs,” she stresses.
As these conditions continue to affect more young and middle aged Kenyans, it is clear that more awareness is needed not just at homes, but also in schools, churches, and even hospitals because tackling NCDs is not just about saving lives, but securing Kenya’s future.














